No 40 - 2012
Bacterial meningitis 2011
Bacterial meningitis 2011
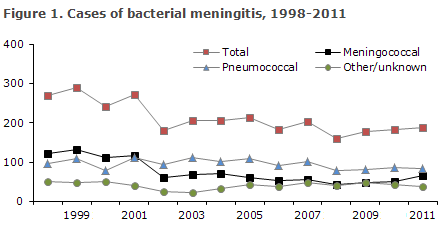
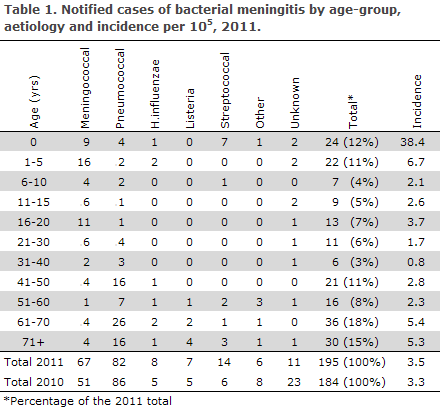
2011 saw a total of 195 notified cases of bacterial meningitis. Figure 1 and Table 1 show the distribution by aetiology and age. Meningococcal meningitis (67 cases) in 2011 is described in EPI-NEWS 38/12.
Pneumococcal meningitis
A total of 82 cases of Streptococcus pneumonia were notified . Among these, 76 were diagnosed by culture, three by PCR and three by microscopy. For 14 patients, information on underlying conditions or dispositions was available: Two were alcohol abusers, two had undergone neurosurgery, two had a dural defect, four had cancer, one was an IV drug user, one had azathioprine-treated Crohn's disease, one had previously undergone a splenectomy and, finally, one had previously had meningitis of unknown aetiology twice.
In 27 cases information on possible infection foci was available: 22 had an otogenic focus and/or sinusitis or other infection of the upper respiratory system and five had pneumonia. Information on sequelae was provided in 60 cases: 13 died and five suffered severe neurological sequelae, including one case of bilateral deafness. Six had cognitive sequelae such as difficulty with concentration or memory, including one with unilateral palsy of the oculomotor nerve. Twelve suffered hearing impairment (including five unilateral cases) and four also had other neurological sequelae. A total of 24 had no sequelae.
Other streptococci
Meningitis due to other streptococci was detected in 14 cases. Group B streptococci were detected in eight cases. Among children under two months of age, including two premature children, a total of four cases of vertical infection were observed along with one case of possible vertical infection.
Two cases were seen in children aged two and four months, respectively, with unknown route of infection. Four children had no sequelae, two suffered hearing impairment, and in one case information on sequelae was unavailable. One fatal case was observed in a 58-year-old patient; there was no information available on underlying conditions or dispositions.
Five cases were caused by group A streptococci: A seven-year-old child with a cochlear implant who suffered no sequelae, and four adults including three for whom information on sequelae had been provided: One died, one suffered no sequelae and one had unilateral hearing impairment. Following a cerebral abscess, S. anginosus meningitis was detected in a 63-year-old patient who suffered cognitive sequelae.
Haemophilus influenzae
Eight cases of H. influenzae were notified. All patients survived. Hib (H. influenzae serotype b) was detected in one unvaccinated three-month-old boy who suffered no sequelae. Serotype f was detected in a 23-month-old girl who suffered no sequelae. Three cases caused by non-capsular H. influenzae were seen in patients aged 45, 70 and 85 years. For another three patients aged two, 54 and 65 years, isolates were not submitted for typing; the 54-year-old patient suffered sequelae in the form of memory impairment; the remaining five had no sequelae.
Listeria monocytogenes
A total of seven cases of meningitis caused by L. monocytogenes were notified, all in patients above 50 years of age. Two were infected in Italy and five in Denmark. Two were immunosuppressed patients with leukaemia, no sequelae; and two had chronic alcohol abuse, no information on sequelae. For one 77-year-old patient, there were no disposing factors or sequelae, while information on dispositions and sequelae was missing for the last two.
Other aetiology
Staphylococcus aureus was detected in three adults: one IV drug abuser, one patient with intraspinal abscess and one for whom no information was available on risk factors. All survived with no sequelae. Escherichia coli was detected in a premature infant who was presumably infected at birth. The infant suffered minor neurological sequelae. Capnocytophaga canimorsus was detected in an asplenic patient for whom no information was avaliable on dog bites or other disposing factors. For this patient, no information on sequelae was provided. Klebsiella pneumoniae was detected in a 58-year male who had previously had otitis media and who suffered sequelae in the form of impaired hearing.
Unknown aetiology
In a total of eleven cases, patients were notified on the basis of clinical tests and investigations and/or cerebrospinal fluid cell counts consistent with bacterial meningitis, but without detection of bacteria by microscopy and culture. All survived and no sequelae were reported.
Commentary
The number of cases of purulent meningitis was roughly in line with that observed in the previous years; 195 cases in 2011 as opposed to 184 in 2010. The slight increase is primarily attributable to an increase in meningococcal meningitis from 51 in 2010 to 67 in 2011. At present, we estimate that this trend has not continued into 2012 (EPI-NYT 38/12). The number of purulent meningitis cases of unknown aetiology decreased from 23 to 11. Meningitis due to other streptococci increased from six in 2010 to 14 in 2011, which is in line with the level observed in 2007 (EPI-NEWS 45/08).
Pneumococcal meningitis decreased from 101 cases in 2007, when the conjugated pneumococcal vaccine was introduced to the childhood vaccination programme, to 82 cases in 2011, EPI-NEWS 37a+b/07. The decrease in pneumococcal meningitis was mainly due to fewer notified cases among children under five years of age, who are covered by the vaccination programme. Thus, the incidence of pneumococcal meningitis in 2011 was 1.5/105 inhabitants compared with 2.9/105/year in 2008-2010 and 5.7/105/year in 2000-2007.
(C. Bjerre, P. Valentiner-Branth, Department of Infectious Disease Epidemiology; T. Dalby, S. Hoffmann, Microbiology and Infection Control)
Link to previous issues of EPI-NEWS
3 October 2012