No 6 - 2014
Rabies prophylaxis
Rabies prophylaxis
In Denmark, being bitten by a bat is normally the only indication for prophylactic treatment against rabies. If, after having been bitten by other animals, there is reason to suspect that the animal has rabies, it should be examined by a veterinary. The veterinary will destroy the animal, if necessary, and arrange further investigation.
In other parts of the world, rabies is more widespread. Transmission occurs through the penetrating bite of an animal infected with rabies or, on rare occasions, through direct contact between infected saliva and mucous membranes or wounds.
The recommendations for post-exposure prophylaxis are available in EPI-NEWS 37/10 where pre- as well as post-exposure prophylaxis is described.
Prophylactic treatment after possible exposure should be discussed with the Department of Infectious Disease Epidemiology, Statens Serum Institut, also outside normal working hours. If post-exposure prophylaxis is indicated, urgent provision of human rabies immunoglobulin (HRIG) and vaccines to GPs may be arranged by Statens Serum Institut at the expense of the Region. Outside normal working hours, HRIG and vaccines can only be supplied urgently to hospitals which themselves cover the costs of HRIG, vaccines and transport. HRIG and vaccines cannot be provided for vaccination clinics and the like.
Post-exposure prophylaxis
In 2013, a total of 148 persons were given prophylactic rabies treatment following animal bites — or other mucous membrane contact — with animals suspected of having rabies, Table 1.
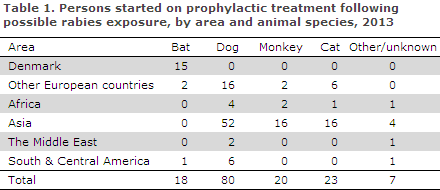
In Denmark, bat bites were the reason why 15 persons received prophylactic treatment, including two children aged one and two years of age. The remaining patients were adults aged between 19 and 65 years.
A total of 14 persons received HRIG as well as vaccination.
One person had previously received pre-exposure vaccination and was therefore given two vaccinations at Day 0 and 3.
For one person, the vaccination series was terminated as the bat in question tested negative for rabies.
A total of 133 Danes were possibly exposed to rabies abroad, 88 in Asia (including 48 in Thailand, seven in Sri Lanka and seven in India), 26 in Europe (including 17 in Turkey), eight in Africa, three in the Middle East and eight in Central and South America, Table 1.
A total of 79 persons received both rabies immunoglobulin (RIG) and vaccination, but in 63 persons, HRIG was only given after they had returned to Denmark. A total of four persons were pre-exposure vaccinated.
Among the 48 persons who were treated following possible rabies exposure in Thailand, 28 had been bitten by dogs, ten bymonkeys, seven by cats and one by a rat, whereas the animal species was unknown/not stated in two cases. Among the 48 persons, two had received pre-exposure vaccination. Among the remaining 46, only six received RIG treatment in Thailand and 36 were vaccinated.
In the remaining 11 of the 12 persons who were treated only after returning to Denmark, exposure occurred from two to 30 days prior to initiation of treatment. In one person who had previously received pre-exposure vaccination, the first of the two vaccines was not given until 52 days after exposure.
Among the 17 persons exposed to rabies in Turkey, 16 were vaccinated, but only one person was treated with RIG in Turkey. Seven received HRIG after returning to Denmark and one person was only treated with HRIG and vaccines ten days after exposure and after having returned to Denmark.
Commentary
In case of bat bites in Denmark, the bat should be caught, if possible, and submitted for rabies testing at the National Veterinary Institute, the Technical University of Denmark, by agreement with the Regional Food Inspectorate.
It is important to follow the occurrence of rabies in Danish bats. The rabies prevalence in Danish bats remains unknown as only a limited number of bats are examined - this was also the case in 2013 when only one of the bats which had bitten a person was examined. If the bat is rabies- negative, the vaccination series is terminated.
Possible exposure to rabies abroad was the primary cause of post-exposure prophylaxis; which was administered to 133 (90%) of all treated persons in 2013. In 2013, a previous pre-exposure rabies vaccination series was reported for five persons.
Patients who have received pre-exposure vaccination and who get bitten by an animal do not need immunoglobulin as they have already produced antibodies, but they should be given two vaccinations; one on Day 0 and the other on Day 3, EPI-NEWS 37/10.
When giving advice prior to foreign travel, it is important to mention the risk of rabies associated with contact to animals. Travellers should be advised to limit contact to animals and to see a physician without delay in case of an animal bite.
Pre-exposure vaccination against rabies may be considered, even in connection with short journeys to rabies-endemic countries. Such vaccination is particularly relevant if the nature of the journey makes it difficult to obtain medical treatment within a few days. It is also important to inform travellers that RIG treatment is unavailable in many parts of the world.
As described, only six out of 46 travellers to Thailand were offered RIG, and the corresponding number for Turkey was one in 16 travellers.
(A.H. Christiansen, S. Cowan, Department of Infectious Disease Epidemiology)
Rabies in animals
Rabies is caused by virus. Two types exist: classic rabies virus and European bat lyssavirus (EBLV), also known as bat rabies virus. Classic rabies is endemic in most of Eastern Europe, while sporadic rabies outbreaks are seen continually in Western Europe, most recently in Italy and Greece. Illegal import of pets from Third-World countries to Europe continues to pose a problem, and 2013 saw several reported cases of rabies in dogs and cats imported from Morocco.
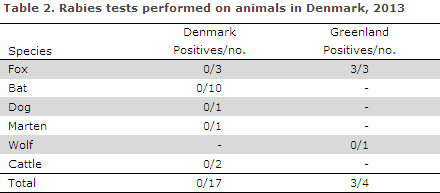
Classic rabies has not been observed in Denmark since 1982, while bat rabies, which is considered to be endemic, was initially detected in 1985. The latest positive finding was seen in a bat in 2009. In 2013 a total of 17 animals were tested for classic rabies virus and/or bat rabies virus, all of which tested negative, Table 2. Classic rabies virus is endemic in Greenland, where Arctic foxes frequently transmit the infection to other mammals. In 2013, classic rabies virus was detected in three Arctic foxes from North Western Greenland, Table 2.
(Thomas Bruun Rasmussen, Virology Section, National Veterinary Institute, Technical University of Denmark)
5 February 2014