No 45 - 2014
Invasive pneumococcal disease and PCV coverage 2013
Invasive pneumococcal disease and PCV coverage 2013
The 7-valent conjugate pneumococcal vaccine (PCV7) was introduced into the Danish childhood vaccination programme on 1 October 2007. The 13-valent conjugate vaccine (PCV-13) was introduced by mid-April 2010. The PCV-7 was phased-out after this date, and 2011 was the first year in which only PCV-13 was administered.
Laboratory monitoring data preceding the introduction of PCV-7 demonstrated that 64% of all cases of invasive pneumococcal disease (IPD) in children up to 5 years of age was caused by pneumococcal serotypes included in the PCV-7 (4, 6B, 9V, 14, 18C, 19F and 23F) and that 91% of IPD in the same age-group was caused by serotypes included in the PCV-13 (the PCV-7 serotypes plus serotypes 1, 3, 5, 6A, 7F and 19A), EPI-NEWS 37a+b /07.
Vaccination coverage
Coverage was calculated using data from the Danish Vaccination Register and included vaccinations administered up to and including 20 August 2014.
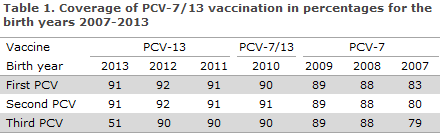
The coverage of the PCV vaccines in the childhood vaccination programme for birth cohorts 2007-2012 was in the 83-92% range for the first PCV, 80-92% for the second PCV and 79-90% for the third PCV, Table 1. For the 2013 birth cohort, vaccination had not been concluded at the calculation date.
Geographical variation was observed, including a slightly lower coverage in the City of Copenhagen, i.e. in the municipalities of Copenhagen, Frederiksberg, Tårnby and Dragør, compared with the remaining parts of the country. For more details, please see www.ssi.dk/data.
Changes in IPD incidence
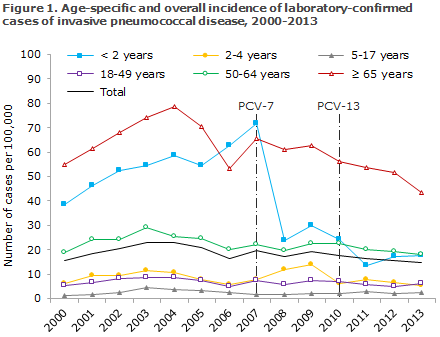
Figure 1 shows the age-specific incidence of laboratory-confirmed IPD cases per 100,000 inhabitants before and after the introduction of PCV-7 and PCV-13 into the childhood vaccination programme.
The report is based on national Danish data from the Neisseria and Streptococcal Reference Laboratory, Statens Serum Institut (SSI).
An IPD case is defined as a disease episode for which pneumococci, Streptococcus pneumoniae, have been cultured in cerebrospinal fluid, blood or another normally sterile sampling material. As from 1 October 2007, submission to the SSI of pneumococcal isolates for serotyping has been required by law to support national monitoring of IPD. In a limited number of cases every year, diagnosis is not made by culture but only by PCR, why serotyping is not always possible.
The overall IPD incidence in the population in the period from 2000 to 2007 before the introduction of PCV vaccination was approx. 20 cases per 100,000 or an average of 1,056 annual cases. This has now been reduced by approx. 20% to 988 annual cases in the PCV-7 period and 869 annual cases in the PCV-13 period.
The decrease in IPD incidence was observed both among vaccinated and unvaccinated age groups. The most pronounced decrease was observed in children < 2 years whose incidence decreased by approx. 71% in the PCV-13 period (2011-2013) compared with the period prior to the introduction of pneumococcal vaccination.
This may therefore be interpreted as the PCV-13 vaccine's efficacy at the population level. Following the introduction of the PCV-13 vaccine, the incidence of the six extra serotypes contained in this vaccine has decreased by 85%. The occurrence of pneumococcal meningitis has also decreased in 2013 to approx. 1/3 of the number observed before the introduction of pneumococcal vaccination, and the reduction has primarily been seen in children below 2 years of age.
Among persons above 65 years of age, a significant decrease in IPD incidence has been seen; from approx. 66 cases per 100,000 in the 2000-2007 period to approx. 50 per 100,000 in 2013. This decrease is mainly owed to a decrease in the occurrence of the serotypes included in the PCV-7 and PCV-13.
The observed decrease in incidence among the elderly, which are most often unvaccinated - the so-called herd effect - is presumably owed to the fact that PCV reduces the carrier state in vaccinated children for the serotypes comprised by PCV and thereby reduces the circulation of vaccine serotypes in the population.
Commentary
Five years after the PCV-7 was introduced, PCV-7 serotypes were hardly observed in IPD isolates from children < 2 years of age in Denmark. PCV-13 has had a corresponding effect on the six extra serotypes. However, data up to and including 2013 show a significant increase in non-vaccine serotypes among children < 2 years of age, and a minor increase in the IPD incidence in this age-group. The increase does not counteract the overall positive effect of the vaccine.
PCV coverage remains approximately one to two percentage points lower than that of the DTaPIPV/Hib and the DTaPIPV/HibHbv vaccine which is given concurrently. The reason for this difference is unknown, but the overall coverage is in line with that observed in previous years, EPI-NEWS 19/13.
(Z.B. Harboe, T. Dalby, H.-C. Slotved, H.B. Konradsen, S. Hoffmann, Microbiology and Infection Control, C.H. Suppli, P.H. Andersen, P. Valentiner-Branth, Department of Infectious Disease Epidemiology)
Link to previous issues of EPI-NEWS
5 November 2014